A previously independent 88-year-old male with no cardiac history was brought to the ED by ambulance at 6.30am with severe chest pain. The pain had come on gradually 45 minutes prior. He had received 300mg aspirin en-route.
On arrival in the resuscitation bay, the patient was in too much distress to give further history.
On examination the patient appeared critically unwell. He was grey and diaphoretic, in severe distress and crying out in pain. GCS 15. Monitoring was attached and revealed non-invasive BP 80/40, HR 80, RR 35, Sat 95% on room air. Narrow complex regular rhythm on cardiac monitor. Breath sounds bilaterally on auscultation of the lungs.
The junior ED registrar (no SMO on-site overnight in this ED) considered the diagnosis of ACS with cardiogenic shock, however was suspicious of the rare but lethal diagnosis of aortic dissection, given the severe pain. Massive PE was considered less likely due to the severity of the pain and lack of hypoxia.
A single ultrasound view of the heart was obtained by the registrar, shown below:
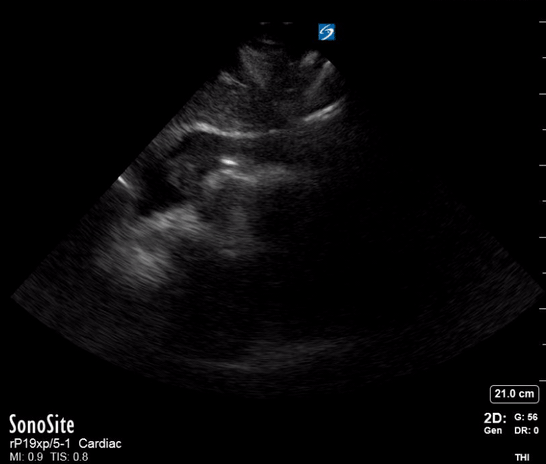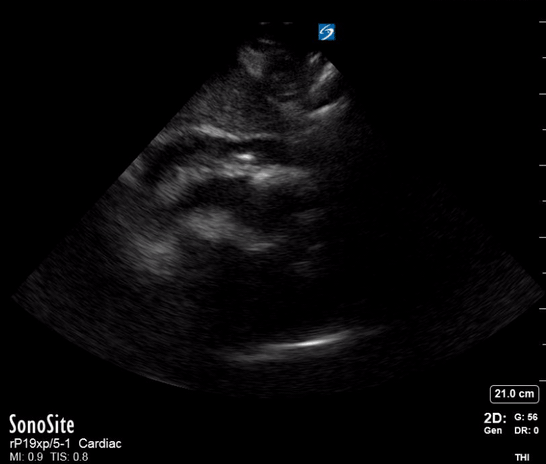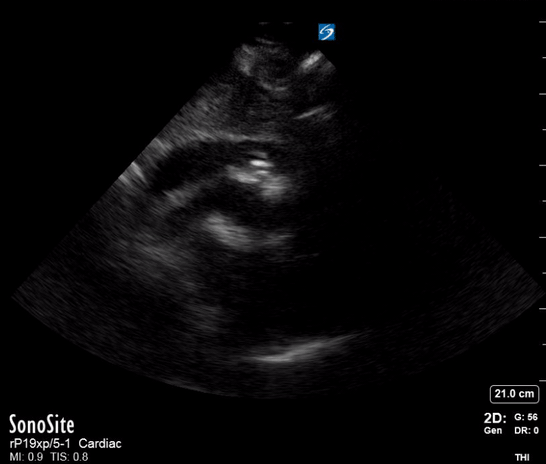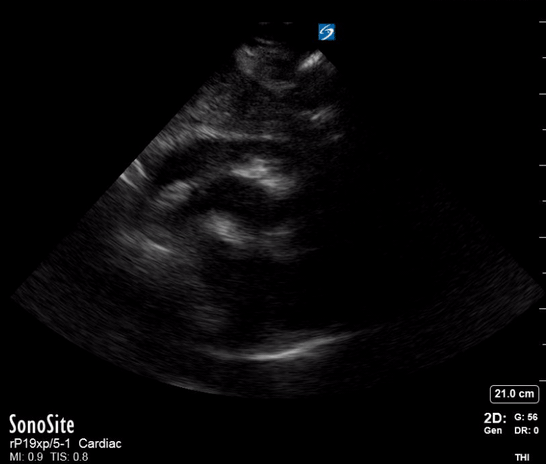
On the basis of the POCUS findings, cardiothoracic surgeons were contacted and the patient was taken urgently to CT, confirming a diagnosis of Type A aortic dissection with large haemopericardium. The patient was taken to the operating theatre for repair. He went into cardiac arrest (PEA, suggesting tamponade as the cause) on arrival in the theatre and underwent sternotomy with internal cardiac massage prior to intubation. The operation then proceeded. He initially made good progress post-op and was discharged from the ICU. Unfortunately he died a week later after an unexplained cardiac arrest on the ward.
What would have happened without POCUS?
There would have been little evidence beyond history to strongly suggest the correct diagnosis in the ED. The textbook finding of Beck’s triad in cardiac tamponade was not useful as the patient did not have distended neck veins, and the presence of “muffled heart sounds” is not a reliable finding in a noisy ED. Without POCUS the patient would likely have waited for a 12-lead ECG and a CXR to be obtained prior to CT being requested, a delay of at least 10 minutes in this time-critical case.

Task-fixation vs. clinical integration of POCUS
Task-fixation is variably defined in the aviation and critical care literature, but generally refers to the inappropriate diversion of attention to a particular sub-activity, at the expense of the overall goal. In other words, “not seeing the forest for the trees”.
Task-fixation in POCUS manifests as a temptation to “complete the examination” or “get better views”, in this case perhaps by obtaining other standard echo windows, or even trying to visualise a dissection flap. This is dangerous because the single, limited-quality view above was sufficient to discount the possibility of ACS or massive PE and assign all clinical resources to pursuing the diagnosis of aortic dissection with tamponade; therefore, more or better views would serve only to delay definitive treatment.
In my experience, task-fixation is a particular risk with POCUS because 1) POCUS is difficult, and 2) POCUS is fun! We all want to achieve good views, especially as learners. It is especially important to avoid in resuscitation or time-critical cases, but should be kept in mind whenever POCUS is performed. Task-fixation can be avoided by ensuring that POCUS is performed with a specific clinical question in mind. Once that question is answered, the exam should stop! This clinical integration is an important way in which POCUS differs from traditional radiology-performed ultrasound.
