A 33-year-old woman presented to the ED with abdominal pain and vomiting. Her symptoms started suddenly, 1 hour after consuming food and 2 standard drinks of alcohol that evening.
There was no blood in the vomit. She reported some PR mucus but no blood. No fever/rigor, no weight loss or odynophagia, no hematuria. She had received IV fentanyl in the ambulance and by the time of her assessment was pain-free.
Her history was notable for Crohn’s disease, diagnosed at biopsy 10 years ago. She had presented to the ED overnight with identical symptoms 3 months prior. At that time she was diagnosed as having an IBD flare and discharged with prednisone and outpatient followup with gastroenterology. The gastroenterologist commented that a flare after 10 years of no symptoms despite being on no medications was unusual, but in the light of raised inflammatory markers, made a plan for MRI of the small bowel.
Her vital signs were normal, afebrile. Examination revealed only mild generalised abdominal tenderness with no extra-abdominal manifestations of IBD.
Urine pregnancy test negative. WCC 15, neutrophils 13, CRP 30, Lipase 103
The treating house officer suspected an alternative pathology and bedside ultrasound was performed.
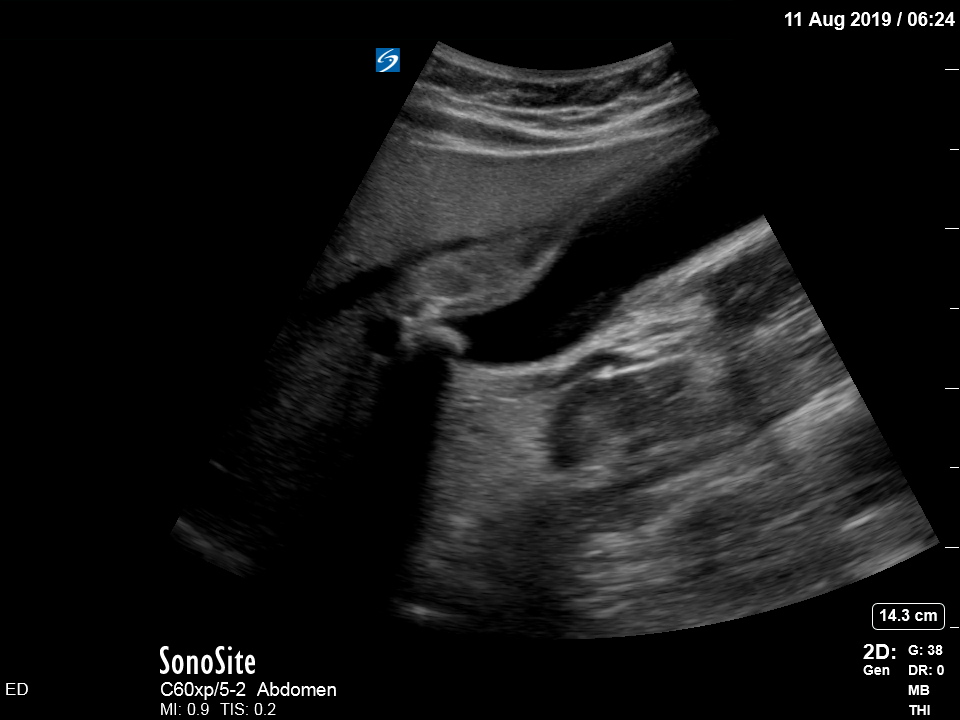
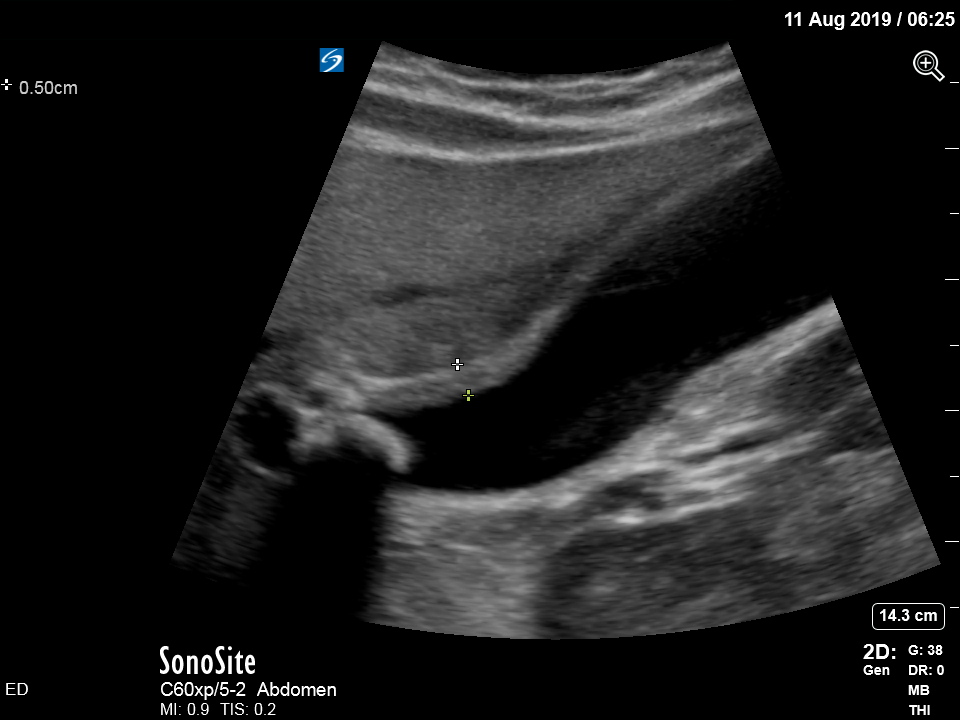
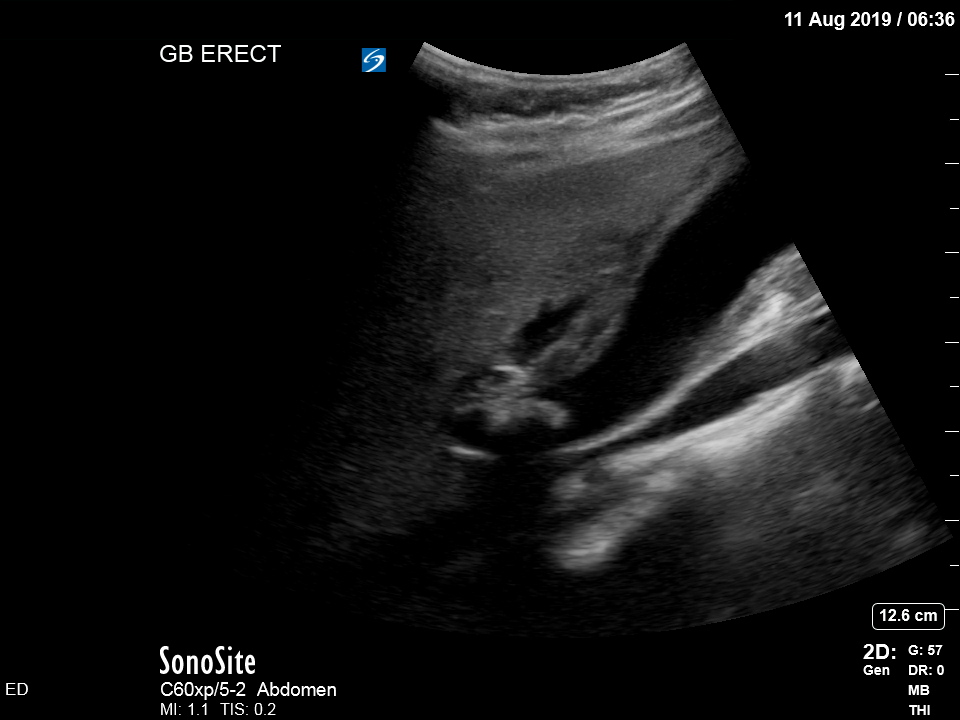
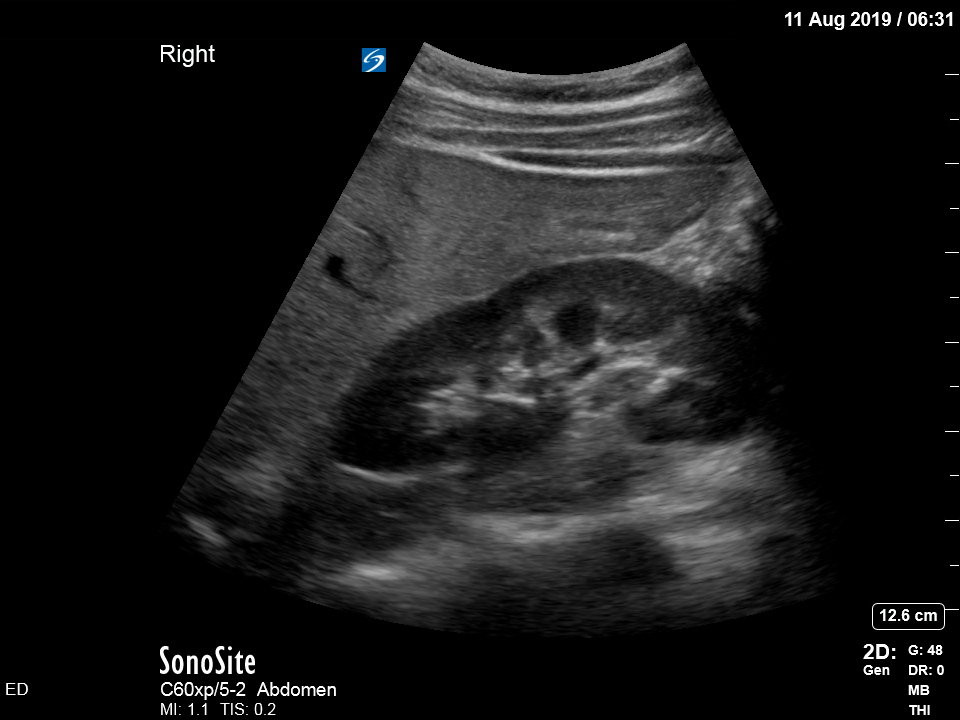
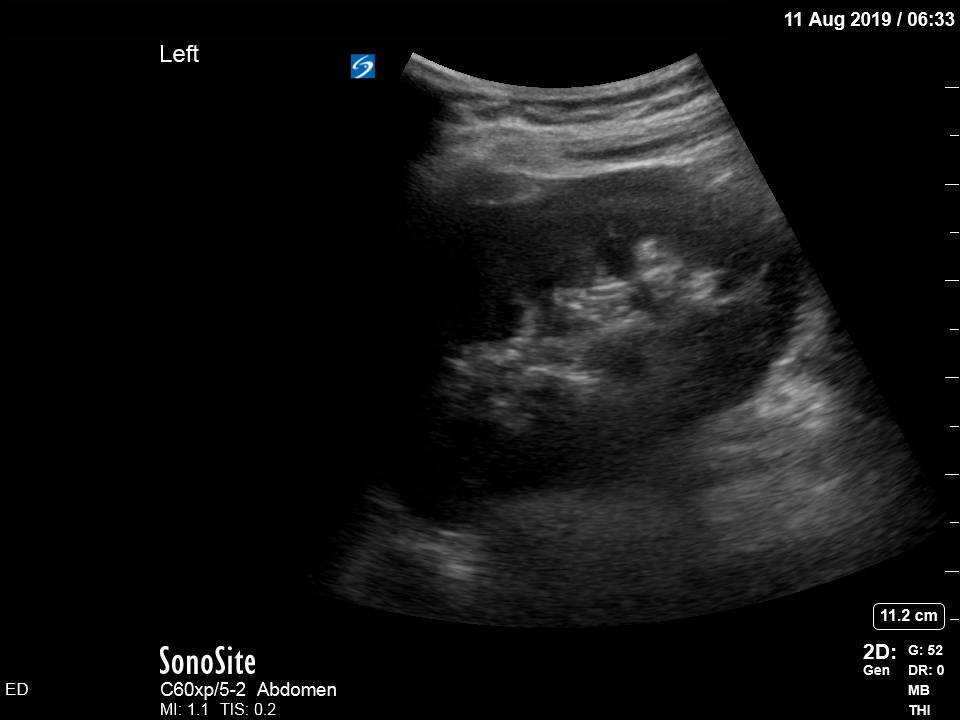
The appearance is typical of acute cholecystitis. The patient was started on IV antibiotics. Images were shown to the surgical registrar who accepted the patient for admission. Formal ultrasound confirmed the findings and the patient went for laparoscopic cholecystectomy within 24hrs. At operation, there was a grossly inflamed gallbladder with an 11mm stone in the neck.
Acute cholecystitis
Ultrasound is the formal imaging study of choice for diagnosing gallstones and acute cholecystitis, which makes it a particularly useful POCUS study. The four sonographic signs of acute cholecystitis are:
- Cholelithiasis (stones in the gallbladder, especially if non-mobile)
- Gallbadder wall thickening (there are various published criteria and rules of thumb but generally >4mm is considered abnormal – though it is more about the edematous/irregular appearance than the specific number)
- Pericholecystic fluid
- Sonographic Murphy sign (the patient is tender when the probe presses on the gallbladder)
Notice the typical appearance of the gallstone – the anterior face reflects ultrasound producing a hyperechoic (bright) surface. Because no sounds waves pass through the stone, the area behind it cannot be imaged and instead we see the artefact known as posterior acoustic shadow.

What would have happened without POCUS?
The patient had a benign abdomen, history of Crohn’s, and recent similar presentation diagnosed as an IBD flare (no POCUS exam was performed). In the absence of clear evidence for an alternative cause, it would have been tempting to again attribute her symptoms to IBD. The tendency to attribute symptoms to an existing diagnosis, without considering alternative options, is an example of anchoring bias.
Without POCUS, she may have again been discharged with steroids, to await her MRI small bowel and gastro followup. Otherwise she may have been admitted under general medicine for steroid therapy and perhaps inpatient MRI/endoscopy. Either way, she would be at risk of developing sepsis from untreated acute cholecystitis.
POCUS helps to overcome cognitive bias and fatigue, by reducing the time and effort required to rule out other causes. Without POCUS, even if considering acute cholecystitis, the only way to rule it out would have been to keep the patient in the department until the morning shift and request a formal ultrasound scan. On a busy night shift in ED, it would have been easy to subconsciously disregard this possibility and avoid having to order an imaging study, making things “easier” for everyone involved.
